AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
Back to Blog
Code book from atlasti3/22/2023 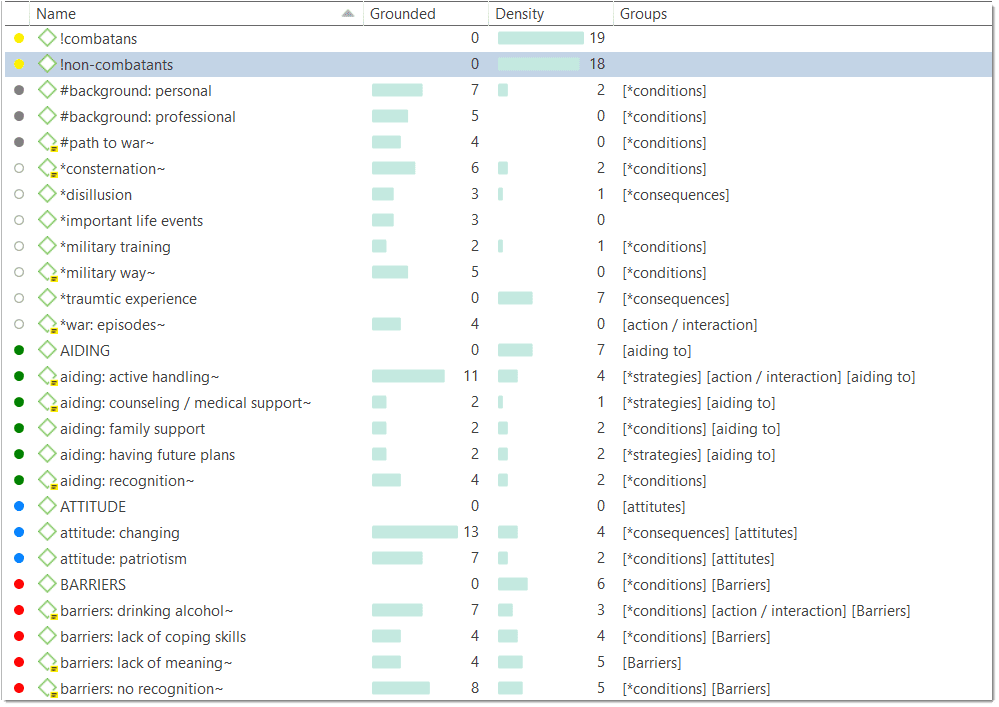 
The frantic preparation and buzzing anticipation that precedes all new emergency admissions plays out daily in intensive care units around the world. Much of the work of the intensive care unit centres around the primary objective of “saving lives”. In addition to the medical complexities involved, negotiation between life and death is also affected by social and cultural influences such as the optimism represented by new biomedical technologies (Morozov, 2013), ongoing professionalization of subspecialities of intensive care (Koch and Checkley, 2017), biopolitical emphases on vitality (Rabinow and Rose, 2006), changing understandings of disease and disability (Hughes, 2015) and political pressure from groups organizing around disability justice and euthanasia (e.g. The application of advanced medical technologies and cutting-edge interventions necessitates a continuous balancing act between maintaining tentative holds on life and facilitating death for the most severely ill and injured patients (Abrams et al., 2014). In many cases, once connections have been made between patients' bodies and the network of life sustaining technologies and medical interventions of the intensive care unit, death only occurs after the deliberate and planned withdrawal of life support allows organ systems to shut down (Mark et al., 2015). After having pulse restored and breathing tube inserted in the emergency department, critically ill patients are rushed to intensive care for continuous monitoring and treatment by a team of nurses, physicians, ventilators, and cardiogenic drugs. 1” If the emergency department is a location for the application of critical first aid and the ritual revival of bodies made possible through cardiopulmonary resuscitation (CPR) (Timmermans, 1999), the intensive care unit represents the assemblage of health professionals and biomedical technologies set up to deal with the bodily care and technological maintenance required next. The practice of intensive care medicine operates somewhere between, “ do everything medically possible” and “ make sure the patient doesn't suffer. Refiguring death as a personal ethical threshold, rather than inherently tragic ending, challenges the power of the logic of lifesaving and instead insists on greater attention towards improving conditions for living. A closer look at how healthcare professionals, medical devices, patients, and families accept, refuse, and modify imposed boundaries of bodily finitude reveals how activities of lifesaving often lead to uncertainty and may even impose harm when they deny possibilities for desired death. Drawing from ethnographic fieldwork and a decade of involvement in clinical research, this paper examines everyday activities of lifesaving in the intensive care unit and interrogates epistemological assumptions upon which they are organized. As a result, the intensive care unit may contribute more towards biopolitical narratives of investment in lifesaving than measurable improvements in population health. However, as the COVID-19 pandemic has demonstrated, intensive care is an expensive, finite resource which is not necessarily available to all citizens, and which may be unjustly rationed. These specialized hospital wards contain the life support machines and technical expertise to sustain seriously ill and injured bodies. 
Intensive care units are considered life-saving medical services and a vital component of healthcare systems.
0 Comments
Read More
Leave a Reply. |
 RSS Feed
RSS Feed
